Period pain is more than just cramps. But for many women the real trouble comes in the lower back; dull, throbbing ache in the lower back that can sometimes spike into sharp pain strong enough to send you home from work or cancel weekend plans. Have you ever noticed that when your lower back is acting up during your cycle, it feels almost impossible to stand up straight or sit comfortably?
You’re not alone.Studies suggest that up to 84% of women experience back pain during their menstrual cycle, making it one of the most common yet least talked-about period symptoms.[1]
Here’s a secret that most people don’t understand: Menstrual pain is not just a uterine issue. It is a reflex that extends well beyond the genitals and an experience, whether looked forward to with excitement or dread, that thrusts you into your body. Understanding why your low back hurts during menstruation, and what you can really do about it, could bring those painful days out of the darkness and into at least a bit of light.
In this article, we’ll decode the real causes of period back pain and practical ways to support your body through your cycle.
Why Does Lower Back Pain Happen During Periods?
Menstrual pain is driven by biochemical and mechanical changes that ripple through your entire body.As your uterus is chugging along during its monthly shedding, many dominoes are being knocked over, and often, your lower back, that poor bastard, takes the brunt of this hormone tango.
Role of Prostaglandins in Period Pain
Prostaglandins are like your body’s chemical messengers that are helpful in moderation but become the enemy when overproduced. These hormone-like compounds are released by your uterine lining to stimulate contractions that allow the body to expel the lining [2]. Here’s where things get uncomfortable:
Prostaglandins trigger uterine contractions ; these contractions are helpful in ridding your body of menstrual tissue, but they can be strong enough to cause pain also. The more prostaglandins your body makes, the heavier and more painful these cramps will be.
They increase pain sensitivity: Prostaglandins aren’t content with simply causing pain, they also actually reduce your threshold for stimuli that hurt elsewhere in your body. That means you’ll feel discomfort more intensely, in places like your lower back [3]..
They affect surrounding muscles: These chemicals don’t remain local to the uterus. They can inflame and tighten the muscles around them, including the ones that help support your spine and pelvis. This develops a chain of effects with pelvic pain transferring to the lower back.
How Hormonal Changes Affect the Lower Back ?
Hormones aren’t just in control of your period, they also impact the way that your muscles, ligaments and even nerves function at different times throughout the month.
Estrogen and Progesterone Fluctuations
A week before and during your period, estrogen and progesterone plummet. Here, how this hormonal change also known as andropause, affects your body in unexpected ways:
They alter pain perception: Progesterone or estrogen levels going down actually make us more of a baby when it comes to feeling pain. Tenderness studies have indicated that the female hormone estrogen has a protective effect on pain perception, so when those levels go down (like in perimenopause), you are more susceptible to acute sensation [4].
They increase ligament laxity: Progesterone, in particular, affects the flexibility of your ligaments and connective tissue. As the levels wax and wane, the supporting ligaments of your spine and pelvis become looser, generating possible instability along with compensatory muscle tension.
They affect posture and stability:These hormonal changes can subtly shift the alignment and stability of your body. Your stabilizers may not fire as efficiently, causing your lower back to work overtime to hold you upright. It’s particularly noticeable if you spend long hours at a desk and/or you already have postural issues.
If you suffer from enduring posture-related discomfort, ergonomic sleeping solutions could offer the essential support that supports your body during these hours of vulnerability.
Can Period Cramps Radiate to the Lower Back?
Absolutely, and it is more common than you might realize. A lot of people think of their lower back as being a separate entity from their uterus, but in truth, they’re intimately connected anatomically.
Referred Pain Explained
Referred pain is the phenomenon of feeling discomfort at a location other than its point of origin. Here’s why it occurs with menstruation:
The uterus shares nerve pathways with the lower back: Nerves exiting the same spinal segments (mostly at T10-L1) may innervate both your uterus and your spine. When your uterus squeezes, the pain signals follow these mutual neural highways [5].
Pain signals spread to the lumbar region: When multiple structures are connected through the same nerve supply, your brain can have a hard time pinpointing exactly where pain is originating. This neurological confusion is why contractions can feel like lower back pain, even when the sensations are being generated in your uterus.
This is why some people feel more back pain than abdominal cramping during their periods, the lines of how your nervous system will route these signals are being drawn differently.
Does Poor Posture Make Period Back Pain Worse?
Yes and here, small adjustments can have a surprisingly big impact.
Why Slouching Intensifies Menstrual Back Pain
When you’re already experiencing hormonal changes and uterine contractions, poor posture is like adding mechanical stress to an open wound:
It increases lumbar compression: The rounding of the low back, or excessive slouching and hunching forward, puts your spine in a mechanically disadvantaged position. This squeezes the lower vertebrae and their tissues which can push on inflammation or spasm provoking agents like prostaglandins.
It reduces circulation: Poor posture decreases the blood supply to your pelvic and lumbar areas. Good circulation is crucial to supplying tissues with the essential oxygen and nutrients they require and removing damaging inflammatory waste products. When you slouch, you are essentially choking off your body’s natural healing power [6].
It tightens hip flexors: Your hip flexors become shortened and tightened when you sit all day, especially if you have crappy posture. These muscles are directly connected to your lumbar spine, and if they’re tight, they’ll pull on your lower back, supplementing strain.
The good news? Properly supporting your body, particularly while you sleep where you spend 7-9 hours in one position, can minimize this mechanical stress. Good orthopedic pillows and supportive mattresses do this by supporting your spine’s natural curvature, minimising the compensatory tension that adds to menstrual back pain.
When Is Period Back Pain Considered Normal?
We all experience some level of discomfort when menstruating, and it’s only normal. But when does it pass over from “uncomfortable, but normal” to something that requires medical attention?
Normal vs Concerning Symptoms
Mild to moderate pain → common: If you have noticeable back pain that doesn’t impede your regular life (except for doing things with some adaptations), this generally falls within what’s expected. You might need to stop and take breaks; use heat therapy or avoid strenuous activities, but you can at least function.
Severe pain disrupting life → needs evaluation: If you have back pain so intense that it causes you to miss work, or school, can’t get out of bed, or requires that you frequently take prescription painkillers then it’s time to see your healthcare provider. This severity of pain might signal such things as:
- Endometriosis: Tissue that lines the uterus grows outside of the uterus, which can be very painful⁷
- Adenomyosis: When the lining of the uterus grows into its muscular wall
- Pelvic inflammatory disease: Infection of the sex organs
- Fibroids: Noncancerous growths either in or on the uterus
Other warning signs include pain that keeps getting worse, pain with a period that’s so heavy you go through a pad or tampon every hour for several hours, or pain that comes at any point during your cycle, not just during menstruation.
Comfort Tips That Actually Help Relieve Period Back Pain
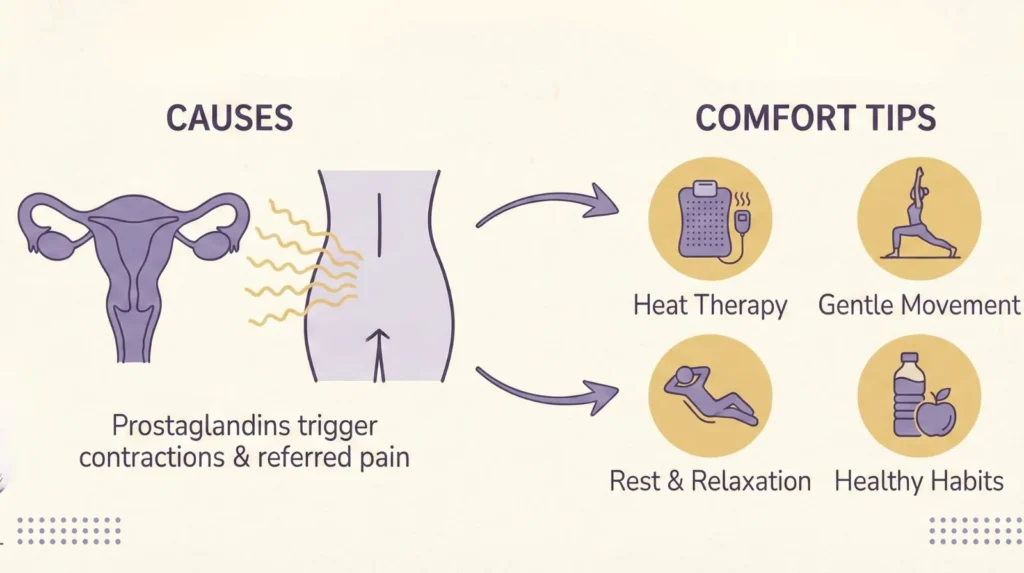
Small adjustments add up and can help you manage or in some cases prevent menstrual back pain. Below are science-based methods that play well with your body’s natural processes.
Effective At-Home Relief Strategies
Heat: Placing something warm/hot on your lower back helps to increase blood flow while relieving tense muscles, and can be comparable to over-the-counter medication for menstrual pain [8]. Apply a heating pad, hot water bottle, or warm bath for 15-20 minutes.
Light stretching: Gentle stretches will help to loosen tension in your lower back, hips and pelvis. Consider cat-cow stretches, child’s pose and easy spinal twists. The operative word is “gentle”; this is not the time for a power yoga class. You are promoting motion and circulation; you’re not testing the limits of your body.
Posture support: Pay attention to how you sit, stand and sleep. Do you use a low back support pillow when seated for extended periods and not slumping? Whilst you rest make sure that your sleep surface is supportive yet not too firm not too soft.
Light movement: Though it may be the last thing in the world you want to do, light activity such as walking or swimming can actually help alleviate menstrual back pain. Physical activity releases endorphins (natural pain killers) and increases blood flow [9]. Even a 10-minute stroll around your local neighborhood can be beneficial.
For relief while you sleep it’s important to have a sleep environment where your body is in perfect alignment. Memory foam and orthopedic pillows that support your spine evenly can help keep your lower back in the right position all night long for a truly restorative sleep.
Is Sleep Position a Factor in Period Back Pain?
Yes, sleep position is more important than many would expect, as during menstruation your body is already handling inflammation and muscle tension.
Best Sleeping Positions During Periods
Back-sleeping with knee support: Sleeping on your back with a pillow under your knees might very well be the most spine friendly position. This position helps you maintain the natural curves in your spine and takes the pressure off of your lower back. The pillow beneath your knees keeps your lower back from arching too much, which may worsen menstrual backaches.
Pillow between knees for side sleeping: If you are a side sleeper, place a pillow between your knees to keep your hips, pelvis and spine in alignment. This action keeps your top leg from yanking on your lower back and hips. Opt for the fetal position with slightly bent knees, this can also help relieve abdominal cramping.
Don’t sleep on your stomach: Sleeping on your stomach will force your neck into an awkward twist and makes the curve of your lower back go backward more than it should. This position is most strenuous on your spine and should be avoided, particularly during your menstrual period.
The building blocks of good sleep posture begin with your mattress and pillow. A supportive bed that holds your spine in line while cradling your pressure points can change everything when it comes to sleeping on during your period. Likewise, selecting the proper pillow height and firmness keeps your head, neck, and spine in a neutral position all night long.
If you have trouble sleeping while on your period, there are several strategies in our guide to better sleep quality that may be useful.
Final Thoughts: Living Comfortably Through Your Cycle
Having lower back pain after period is not “just something to deal with.” Understanding the hormonal, muscular and postural factors behind it allows for smarter, gentler relief that works with your body, not against it.
The secret is dealing with all of these factors at once: controlling inflammation with heat and gentle motion, maintaining correct posture during the day, and sleeping in an environment that supports proper alignment for recovery each night.
But remember: Your menstrual cycle is a natural process, though debilitating pain ought not be. By melding evidence-based self-care practices with correct postural support, you can win back those days that were once spent as ‘pain days’.
How Betterhood Helps You Live Pain-Free
We know at betterhood that comfort is more than a luxury and instead, it’s the cornerstone of living well. Durable Support for Body During Sleep, Our posture-perfect wellness tools keep your lower back supported whether you’re resting, relaxing or recovering and every night during menstruation.
Cheerful support, in the form of orthopedic pillows that maintain your cervical curve to pressure-relieving mattresses supporting your spine’s natural curves, can make unbearable days feel a little easier and less like a sentence.
Because we all deserve to wake up refreshed and never held back by pain.
Explore More Health & Wellness Solutions:
Would you like to be up-to-date on everyday health and wellness issues? Here are some interesting pieces to help you. Follow the links below if you want practical tips or solutions:
- What Causes Back Pain? Understanding Root Triggers & Prevention Tips
- 10 Effective Home Remedies for Body Pain Relief Naturally
- Wrist Support Braces Explained: Protocols for Pain Relief
- Chronic Shoulder Pain due to Frozen Shoulder : Understanding the Cause
Frequently Asked Questions
Yes. Period back pain is relatively common, thanks to the fact that prostaglandins, hormones and uterine contractions can force your muscles to work harder (most women don’t know this so they suffer in silence but it’s a truth), but severe pain should be addressed by a provider.
This is called referred pain. Your uterus and lower back share nerve pathways, so uterine cramps can feel like back pain. Some people feel it more in the back than the abdomen.
Yes. Bad posture puts pressure on your spine and tension in the pelvis that can exacerbate period back pain.
Sleep on your back with a pillow under your knees or on your side with a pillow between them. Spinal alignment is supported by both positions and the lower back is relieved of tension.
Seek medical assistance if the pain is severe, getting worse, occurs outside of periods or with heavy bleeding or fever and unusual discharge.
Yes. Light activity like walking or stretching increases blood flow and endorphins, which can ease period back pain.
References
- Mayo Clinic. (2023). Menstrual cramps: Symptoms and causes. Retrieved from https://www.mayoclinic.org/diseases-conditions/menstrual-cramps/symptoms-causes/syc-20374938
- Cleveland Clinic. (2023). Dysmenorrhea (painful periods): Overview. Retrieved from https://my.clevelandclinic.org/health/diseases/4148-dysmenorrhea
- Iacovides, S., Avidon, I., & Baker, F. C. (2015). What we know about primary dysmenorrhea today: A critical review. Human Reproduction Update, 21(6), 762-778. https://doi.org/10.1093/humupd/dmv039
- Harvard Health Publishing. (2022). Hormones and pain sensitivity. Harvard Medical School. Retrieved from https://www.health.harvard.edu/pain/hormones-and-pain-sensitivity
- NHS. (2022). Period pain: Causes and symptoms. National Health Service. Retrieved from https://www.nhs.uk/conditions/period-pain/
- Waller, B., Lambeck, J., & Daly, D. (2009). Therapeutic aquatic exercise in the treatment of low back pain: A systematic review. Clinical Rehabilitation, 23(1), 3-14. https://doi.org/10.1177/0269215508097856
- American College of Obstetricians and Gynecologists. (2023). Endometriosis: FAQ. Retrieved from https://www.acog.org/womens-health/faqs/endometriosis
- Akin, M. D., Weingand, K. W., Hengehold, D. A., Goodale, M. B., Hinkle, R. T., & Smith, R. P. (2001). Continuous low-level topical heat in the treatment of dysmenorrhea. Obstetrics & Gynecology, 97(3), 343-349. https://doi.org/10.1016/s0029-7844(00)01163-7
- Daley, A. J. (2008). Exercise and primary dysmenorrhoea: A comprehensive and critical review of the literature. Sports Medicine, 38(8), 659-670. https://doi.org/10.2165/00007256-200838080-00004


















